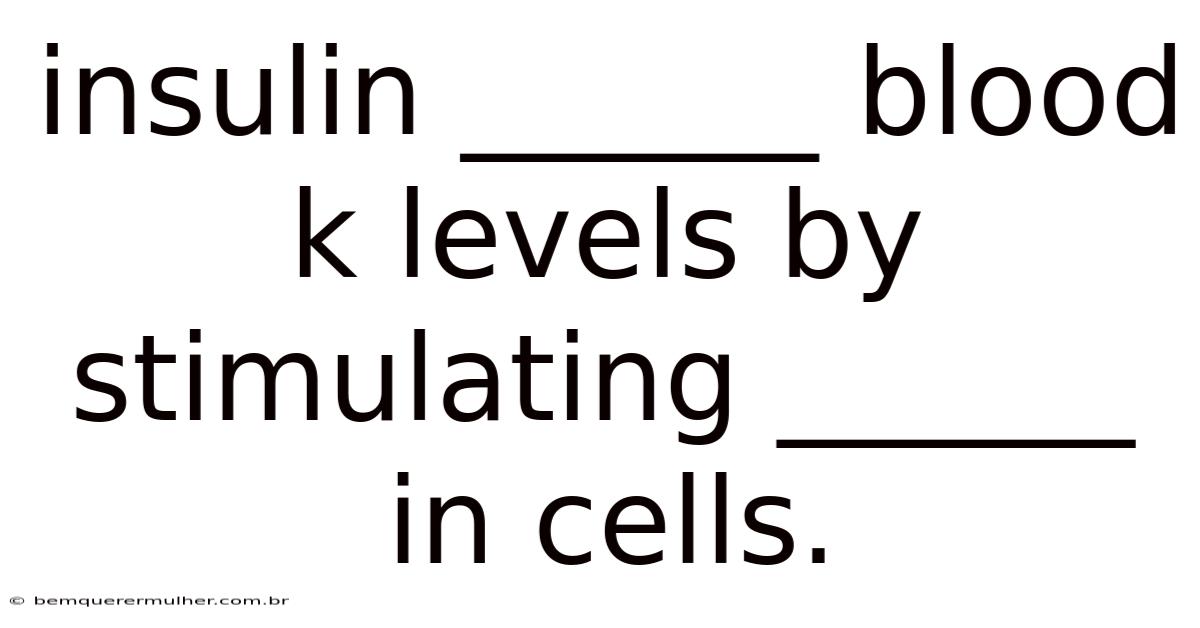The human body operates as a finely tuned orchestra where every instrument plays a critical role in maintaining harmony. That's why within this involved system lies a vital component—insulin—that acts as the conductor, orchestrating the flow of nutrients through the bloodstream. Because of that, insulin’s function extends beyond mere regulation; it is a cornerstone of metabolic balance, directly influencing blood glucose levels and ensuring cellular energy demands are met. When insulin levels fluctuate, the consequences can ripple through every system, from energy production to organ function. Understanding the dynamics of insulin’s impact is essential for grasping its profound significance in health, disease, and longevity. Think about it: this article gets into the mechanisms by which insulin stimulates cellular processes, explores the physiological implications of its action, and examines its role in addressing contemporary health challenges. By examining these facets, readers will gain insight into how a single hormone can serve as a bridge between biological complexity and practical application, offering clarity in an era where misinformation often overshadows scientific truth.
The Role of Insulin in Glucose Regulation
Insulin’s primary function is to help with the uptake of glucose into cells, thereby lowering blood glucose concentrations. This process occurs predominantly in peripheral tissues such as muscle, fat, and liver cells, where glucose is stored or converted into glycogen for later use. On the flip side, insulin’s influence extends beyond mere absorption; it triggers a cascade of metabolic responses that ensure cells can access energy efficiently. Here's one way to look at it: when blood sugar levels rise post-meal, insulin acts as a signal, prompting cells to absorb glucose through the conversion of glucose to glycogen or its utilization for ATP production. This mechanism not only stabilizes immediate energy needs but also signals the body to prioritize glucose utilization over other processes. Conversely, elevated blood glucose levels—such as those seen in diabetes—demand heightened insulin secretion, highlighting its dual role as both a regulator and a responder. The interplay between insulin and glucose is thus a dynamic equilibrium, where deviations from balance can lead to metabolic disorders, emphasizing insulin’s centrality to homeostasis.
Cellular Stimulation: The Mechanism Behind Insulin Action
The stimulation of cellular response by insulin involves a series of molecular interactions that unfold within cells. At the cellular level, insulin binds to specific receptors on target cells, initiating a signaling cascade that culminates in the activation of key enzymes responsible for glucose transport. This process begins with the translocation of GLUT4 transporters to the cell membrane, a phenomenon particularly prominent in skeletal muscles and adipose tissue. These transporters allow the movement of glucose into the cytoplasm, where it is metabolized into pyruvate or utilized directly for energy production. Additionally, insulin stimulates the production of insulin-independent glucose-producing pathways, such as gluconeogenesis in the liver, ensuring a sustained supply of energy reserves. The efficiency of this process is further enhanced by insulin’s ability to modulate insulin sensitivity, allowing cells to respond more effectively to the hormone’s presence. Such cellular-level adjustments underscore insulin’s versatility, positioning it as a multifaceted regulator that adapts to both acute and chronic physiological demands Practical, not theoretical..
Insulin’s Impact on Metabolic Pathways
Beyond glucose uptake, insulin influences broader metabolic networks, including lipid metabolism and protein synthesis. By promoting the storage of excess glucose as glycogen or fat, insulin curtails the breakdown of these stores, preserving energy reserves. Simultaneously, it suppresses the synthesis of non-essential proteins, redirecting amino acids toward essential functions rather than accumulating waste products. This dual action not only stabilizes blood glucose but also safeguards against fat accumulation, a critical factor in preventing conditions like obesity and type 2 diabetes. Adding to this, insulin’s role in adipose tissue regulation extends to its influence on adipocyte differentiation, ensuring that fat storage remains in check. These interconnected effects illustrate how insulin acts as a central hub, orchestrating pathways that collectively maintain metabolic equilibrium. Understanding these pathways reveals the depth of insulin’s influence, positioning it as a linchpin in sustaining metabolic health Simple, but easy to overlook..
Addressing Insulin Resistance and Its Consequences
Despite its widespread importance, insulin resistance—a condition where cells become less responsive to insulin—poses a growing public health concern. In this state, the body struggles to efficiently transport glucose into cells, leading to elevated blood sugar levels despite elevated insulin concentrations. This paradox underscores the complexity of insulin’s role, as resistance often stems from altered receptor function, impaired signaling, or disrupted cellular communication. Consequences of insulin resistance include hyperglycemia, increased risk of cardiovascular disease, and progressive loss of muscle mass, exacerbating metabolic dysfunction. Addressing this challenge requires multifaceted strategies, including dietary modifications, exercise regimens, and pharmacological interventions designed to restore insulin sensitivity. Such approaches highlight the necessity of a holistic understanding of insulin’s role, as well as the urgency of developing targeted therapies that mitigate its adverse effects while preserving its essential functions.
Insulin’s Role in Disease Prevention and Management
The relationship between insulin levels and disease prevalence further illustrates its significance in public health. Conditions such as type 1 diabetes, characterized by insufficient insulin production, and type 2 diabetes, marked by insulin resistance, serve as stark examples of insulin’s central role in metabolic control. Beyond these, insulin dysfunction also contributes to non-alcoholic fatty liver disease, metabolic syndrome, and even neurodegenerative disorders, where disrupted glucose homeostasis impacts brain function. Conversely, maintaining optimal insulin sensitivity through lifestyle adjustments—such as balanced nutrition, regular physical activity, and stress management—can significantly reduce the risk of developing these conditions. Worth adding, emerging research suggests that insulin-like growth factors (IGFs) may play complementary roles in promoting cellular repair and longevity, further expanding insulin’s therapeutic potential. These insights reinforce the importance of monitoring and managing insulin levels as a proactive strategy for preventing or mitigating associated health complications That's the part that actually makes a difference..
The Synergy of Insulin and Cellular Adaptation
Cellular adaptation to insulin’s influence is a testament to the body’s resilience and adaptability. Over time, chronic exposure to elevated insulin levels can lead to cellular exhaustion, where insulin signaling pathways become dysregulated.
This cellular exhaustion manifests through several interconnected mechanisms, including downregulation of insulin receptors, accumulation of inflammatory mediators, and mitochondrial dysfunction. As cells become increasingly overwhelmed, the compensatory hyperinsulinemia that initially maintained glucose homeostasis eventually fails, precipitating the full-blown metabolic derangements characteristic of advanced insulin resistance.
On the flip side, the body employs remarkable adaptive strategies to mitigate these effects. Autophagy, the cellular recycling process, has a big impact in clearing damaged components and restoring metabolic balance. Similarly, the upregulation of insulin-like growth factor binding proteins helps modulate insulin-like signaling, providing alternative pathways for glucose utilization when classical insulin signaling becomes compromised. These adaptive mechanisms underscore the complex feedback loops that govern metabolic homeostasis, though they ultimately prove insufficient when faced with sustained physiological stress Practical, not theoretical..
The therapeutic implications of understanding these adaptive processes are profound. Rather than simply targeting blood glucose levels, modern treatment approaches increasingly focus on restoring cellular sensitivity to insulin through multiple modalities. That said, gLP-1 receptor agonists, for instance, not only enhance insulin secretion but also promote weight loss and reduce inflammatory markers, addressing the underlying drivers of insulin resistance. Meanwhile, SGLT2 inhibitors work by increasing glucose excretion, effectively lowering the metabolic burden on insulin-resistant cells.
Looking toward the future, personalized medicine holds promise for more nuanced insulin management. Genetic profiling can identify individuals at higher risk for insulin dysfunction, enabling early intervention before clinical manifestations develop. Additionally, advances in continuous glucose monitoring technology empower patients with real-time insights into their metabolic responses, facilitating more informed lifestyle decisions and treatment adjustments That alone is useful..
All in all, insulin's role in human health extends far beyond its classical function as a glucose-regulating hormone. Worth adding: understanding the delicate balance between insulin sensitivity and resistance—along with the body's adaptive responses to metabolic stress—remains essential for developing effective strategies to combat the growing burden of metabolic disease worldwide. It serves as a central integrator of metabolic, cardiovascular, and cellular processes, with profound implications for disease prevention and treatment. As research continues to unravel the complexities of insulin signaling and its broader physiological effects, the potential for novel therapeutic interventions and preventive measures grows increasingly promising, offering hope for improved health outcomes across diverse populations The details matter here..